How to Build HIPAA-Compliant AI Voice Agents for Healthcare
Table of Contents
Subscribe To Our Newsletter

In a Nutshell
Building HIPAA-compliant AI voice agents for healthcare is not just about adding voice automation to patient calls. It requires a secure, workflow-first approach where every conversation, data point, vendor, system integration, and AI response is designed around privacy, compliance, and patient safety.
- Start with a clear healthcare workflow, not the AI model.
- Map every place where PHI is created or shared.
- Choose a secure architecture with compliance built into every layer.
- Use healthcare-ready speech-to-text, NLP, and agent orchestration tools.
- Verify patient identity before sharing any sensitive health information.
- Set strict guardrails so the AI does not give unsafe advice.
- Protect data with encryption, access control, logs, and retention rules.
- Work only with vendors that support BAAs and HIPAA requirements.
- Integrate with EHR and EMR systems using least-privilege access.
- Keep humans involved for clinical, uncertain, or high-risk conversations.
Healthcare conversations are rarely simple. A patient may call to book an appointment, confirm insurance, ask about lab results, request prescription support, or explain symptoms that need urgent attention. Meanwhile, clinics and hospitals need faster documentation, lower call pressure, and better after-hours support.
This is where HIPAA-compliant AI voice agents become valuable. They can understand spoken requests, respond naturally, route calls, capture information, transcribe conversations, and trigger workflows.
But in healthcare, convenience is not enough. Any voice AI system handling protected health information must be built with privacy, security, auditability, and compliance from day one.
What Is a HIPAA-Compliant AI Voice Agent?

A HIPAA-compliant AI voice agent is an AI-powered voice system designed to communicate with patients, providers, or staff while protecting electronic protected health information, commonly known as ePHI.
It can understand spoken language, process healthcare-specific requests, respond through natural voice, and connect with clinical or administrative systems. But the important part is not just the voice interaction. The system must be built with safeguards that control how patient data is collected, processed, stored, transmitted, accessed, logged, retained, and deleted.
In simple terms, a healthcare voice AI agent should be able to:
- Answer patient calls securely
- Verify identity before sharing sensitive information
- Collect only necessary information
- Route urgent cases to human staff
- Create call summaries or notes
- Transcribe medical conversations
- Integrate with EHR or EMR systems
- Maintain access logs and audit trails
- Encrypt data during transfer and storage
- Work only with vendors that support healthcare compliance
This makes HIPAA-compliant voice AI solutions different from ordinary voice bots used in retail, banking, travel, or customer support. Healthcare voice systems deal with sensitive information such as appointment history, symptoms, medications, diagnoses, insurance details, clinical notes, and patient identifiers.
That means the AI agent must be designed around privacy first, not added later as a security patch.
Build Voice AI That Patients Can Trust
Create secure healthcare voice agents that simplify calls, appointments, documentation, and patient support with confidence.
How to Build HIPAA-Compliant AI Voice Agents for Healthcare
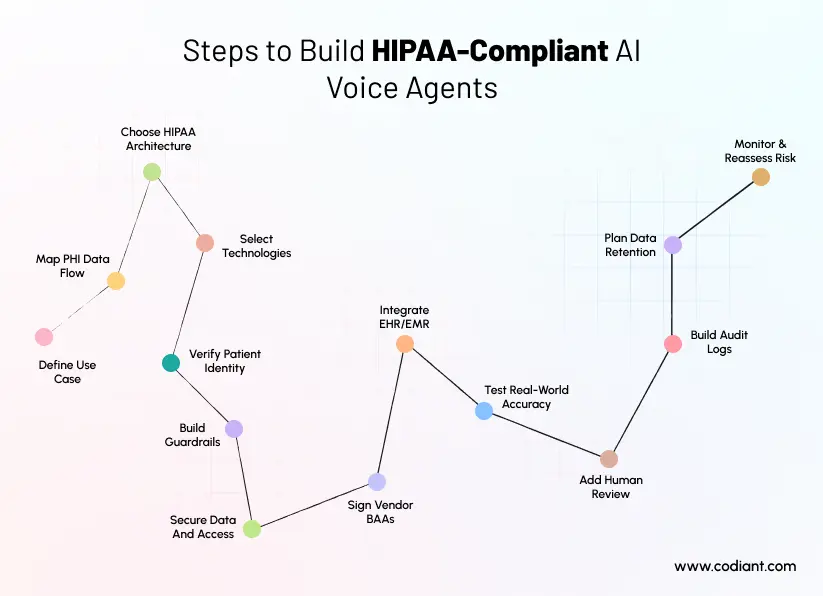
Building HIPAA-compliant AI voice agents requires a structured development process. You need to combine product planning, conversational AI, healthcare integrations, security engineering, compliance documentation, and continuous monitoring.
Here is a practical roadmap.
Step 1: Define the Healthcare Use Case Clearly
Do not start with the model. Start with the workflow.
A voice AI agent for appointment booking is very different from a medical transcription assistant. A post-discharge follow-up bot is different from a nurse triage support tool. A front-desk voice agent may need scheduling access, while a clinical documentation agent may need secure transcription and note generation.
Start by defining:
- Who will use the agent?
- Patients, providers, nurses, front-desk staff, administrators, or billing teams?
- What conversation will it handle?
- What data will it collect?
- What systems will it access?
- Will it handle PHI or ePHI?
- When should it escalate to a human?
- What should it never answer?
- What should it log?
- What should it delete?
For example:
Use Case: Appointment Scheduling Agent
The AI agent handles inbound patient calls, verifies basic identity, checks provider availability, books appointments, sends confirmations, and routes urgent symptoms to staff.
Use Case: Medical Transcription Agent
The AI captures provider-patient conversations, converts speech to text, generates structured summaries, and sends draft notes to a clinician for review.
Use Case: Post-Discharge Follow-Up Agent
The AI calls patients after discharge, asks approved follow-up questions, captures responses, flags concerning answers, and alerts care teams.
Each use case requires different data access, different risk levels, and different compliance controls.

Step 2: Map PHI and Data Flow
Before selecting tools, map every point where patient information enters, moves, transforms, and exits the system.
For a healthcare voice AI system, data may flow through:
- Phone call audio
- Speech-to-text engine
- Natural language understanding layer
- AI model or agent framework
- Conversation memory
- Backend application server
- EHR or EMR API
- CRM or scheduling system
- Database
- Analytics dashboard
- Call recording storage
- Notification system
- Human handoff console
- Logs and monitoring tools
This step is critical because healthcare teams often secure the main database but forget about secondary places where sensitive data appears, such as debug logs, transcripts, model prompts, call recordings, analytics exports, or support dashboards.
A HIPAA-focused data flow map should answer:
- Where is ePHI created?
- Where is it stored?
- Where is it transmitted?
- Which vendors touch it?
- Is it encrypted?
- Who can access it?
- How long is it retained?
- Can it be deleted?
- Is it used for model training?
- Is it shared with any third party?
- Is there a signed business associate agreement where required?
This becomes the foundation for risk analysis, system architecture, vendor selection, and compliance review.
Step 3: Choose a HIPAA-Ready Architecture
A strong architecture for medical voice assistant development should separate the voice layer, AI reasoning layer, healthcare workflow layer, data layer, and compliance layer.
A typical architecture may include:
Voice Input Layer
This handles phone calls, audio streaming, call routing, telephony, and voice capture.
It may include:
- SIP trunking
- VoIP integration
- Contact center integration
- Call recording controls
- Real-time audio streaming
- Voice activity detection
Speech-to-Text Layer
This converts spoken words into text.
For healthcare speech-to-text AI, accuracy matters because medical words, drug names, dosage details, provider names, and patient symptoms can be misheard. The system should support medical vocabulary, noise handling, speaker diarization, and confidence scoring.
Natural Language Understanding Layer
This identifies the caller’s intent.
Examples:
- Book appointment
- Cancel appointment
- Ask billing question
- Request prescription refill
- Report symptom
- Ask for lab result
- Speak to staff
- Confirm insurance
AI Agent Orchestration Layer
This is where the agent decides what to do next. It may call APIs, ask follow-up questions, retrieve allowed information, create a task, update a record, or escalate the conversation.
Healthcare Workflow Layer
This connects the AI voice agent to scheduling systems, EHR/EMR platforms, billing tools, CRM systems, patient portals, and care management platforms.
Security and Compliance Layer
This includes encryption, access controls, identity verification, audit logs, consent handling, monitoring, anomaly detection, data retention controls, and administrative policies.
Human Handoff Layer
Healthcare voice AI should never operate without escalation paths. The system should route calls to staff when there is uncertainty, urgency, sensitive information, patient distress, complex clinical discussion, or policy limitations.
This architecture keeps the AI agent useful while preventing it from becoming uncontrolled.
Did You Know?
The global market for AI voice agents in healthcare was valued at USD 468 million in 2024 and is expected to reach USD 3.18 billion by 2030. North America currently leads the market, while most healthcare voice AI systems are being deployed through cloud-based platforms.
Step 4: Select the Right Technologies
The technologies required for healthcare voice AI development depend on the use case, but most systems include the following components.
- Telephony and Voice Infrastructure
This allows the AI agent to make and receive calls.
Key capabilities:
- Inbound and outbound calling
- Call transfer
- Call recording control
- Real-time streaming
- Failover routing
- Queue management
- Integration with existing phone systems
- Speech-to-Text Engine
The speech-to-text layer converts audio into text for processing.
Healthcare-specific requirements include:
- Medical vocabulary support
- Accent and dialect handling
- Speaker separation
- Noise reduction
- Low-latency transcription
- Confidence scoring
- Custom terminology support
- Secure processing
This is essential for healthcare speech-to-text AI and AI-powered medical transcription use cases.
- Natural Language Processing
NLP helps the AI understand patient intent, extract required entities, and guide the conversation.
For example:
- Patient name
- Date of birth
- Appointment date
- Provider name
- Symptoms
- Medication names
- Insurance details
- Urgency indicators
- Large Language Model or Conversation Engine
The LLM or conversation engine generates responses, summarizes calls, handles context, and supports natural conversations.
For healthcare, the model should be controlled with:
- Strict system prompts
- Retrieval boundaries
- Guardrails
- Approved response templates
- Human escalation rules
- PHI masking
- No unauthorized training on patient data
- Conversation memory limits
- Agent Framework
An agent framework helps the system perform actions, not just answer questions.
It can:
- Check availability
- Book appointments
- Update records
- Create tickets
- Trigger reminders
- Send summaries
- Route calls
- Query approved databases
- Escalate to staff
This is what turns a voice assistant into an operational healthcare agent.
- EHR and EMR Integration Layer
Many healthcare voice agents need to work with EHR or EMR systems.
Common integration needs include:
- Patient lookup
- Appointment scheduling
- Provider availability
- Visit summaries
- Documentation export
- Lab status lookup
- Billing data lookup
- Secure messaging
- Referral management
Integration should be API-based, permission-controlled, logged, and tested carefully.
- Secure Database and Storage
The system may store:
- Conversation transcripts
- Audio recordings
- Call summaries
- Appointment data
- Audit logs
- Consent records
- Task status
- User access records
Storage should support encryption, retention policies, access controls, backup, and deletion workflows.
- Monitoring and Analytics
Monitoring helps track system performance, safety, and compliance.
Important metrics include:
- Call completion rate
- Escalation rate
- Transcription accuracy
- Intent recognition accuracy
- Average handling time
- Error rates
- Patient satisfaction
- Unauthorized access attempts
- Failed authentication attempts
- PHI exposure risks
- Human override frequency
- Compliance Documentation
The system should maintain documentation for:
- Risk analysis
- Vendor review
- Data flow diagrams
- Security controls
- Incident response plan
- Access policies
- Retention policy
- Audit logs
- Business associate agreements
- Testing reports
This is important because HIPAA compliance is not only about having secure code. It is also about proving that the organization has reasonable and appropriate safeguards.
Step 5: Design Secure Patient Identity Verification
Voice AI systems should not disclose sensitive information just because someone knows a patient’s name.
Identity verification should match the sensitivity of the requested action.
For low-risk actions, such as general clinic hours, verification may not be required.
For medium-risk actions, such as appointment confirmation, the system may verify:
- Name
- Date of birth
- Phone number
- Appointment reference
For high-risk actions, such as lab result discussion, medication information, or insurance details, stronger verification may be needed.
Options include:
- One-time passcodes
- Patient portal authentication
- Registered phone verification
- Security questions
- Staff handoff
- Multi-factor authentication for staff dashboards
The AI agent should also be trained not to reveal sensitive information in voicemail, shared phone environments, or uncertain identity situations.
Step 6: Build HIPAA-Focused Conversation Guardrails
Healthcare conversations need boundaries.
An AI voice agent should not behave like an open-ended medical advisor unless it has been specifically designed, validated, and approved for that purpose. In many cases, the safest approach is to keep the agent focused on administrative support, documentation assistance, and approved patient workflows.
Guardrails may include:
Scope Control
The agent should know what it can and cannot do.
For example:
Allowed:
- Schedule appointments
- Confirm visit details
- Collect intake information
- Send reminders
- Capture refill requests
- Generate call summaries
Not allowed:
- Diagnose medical conditions
- Recommend prescription changes
- Interpret complex lab results without clinician review
- Replace emergency care
- Give unsupported clinical advice
Approved Language
For sensitive topics, responses should be pre-approved.
Example:
“I can help collect your concern and notify the care team. If this is a medical emergency, please call emergency services or visit the nearest emergency department.”
Escalation Triggers
The system should escalate when it detects:
- Chest pain
- Severe breathing difficulty
- Suicidal language
- Stroke-like symptoms
- Pregnancy complications
- Medication reaction
- Pediatric emergency
- Confusion or unclear identity
- Repeated misunderstanding
- Patient frustration
- Low transcription confidence
Confidence Thresholds
If the system is not confident, it should not guess. It should clarify, repeat, or transfer.
PHI Redaction
Transcripts, logs, analytics, and model prompts should avoid exposing unnecessary PHI. Sensitive details can be masked where possible.
Step 7: Secure Data Storage, Transmission, and Access
Security must be built across the full system.
For HIPAA-compliant voice AI solutions, common technical safeguards include:
- Encryption in transit
- Encryption at rest
- Role-based access control
- Unique user IDs
- Strong authentication
- Audit logs
- API access controls
- Secure key management
- Session timeout
- Backup encryption
- Network segmentation
- Data loss prevention
- Vulnerability scanning
- Penetration testing
- Environment separation
- Production access restrictions
In January 2025, HHS proposed updates to strengthen HIPAA Security Rule cybersecurity protections for ePHI, including areas such as multifactor authentication, encryption, network segmentation, risk analysis, compliance documentation, and incident response planning; these were proposed changes, not a final rule at the time of publication.
Even where a control is not explicitly mandatory in every current scenario, many healthcare organizations treat these practices as baseline expectations because healthcare data is a high-value target.
A secure AI voice agent in healthcare should also control how data appears in prompts and responses. If a language model receives patient data, that interaction must be governed. The vendor relationship, data processing terms, retention rules, logging settings, and model training policies all matter.
Step 8: Sign Business Associate Agreements with Vendors
If a third-party vendor creates, receives, maintains, or transmits PHI on behalf of a covered entity, a Business Associate Agreement may be required.
For voice AI, vendors may include:
- Telephony providers
- Cloud hosting providers
- Speech-to-text providers
- LLM providers
- EHR integration vendors
- Analytics providers
- Support desk tools
- Call recording platforms
- Monitoring tools
- Data storage providers
Each vendor should be reviewed for:
- HIPAA support
- BAA availability
- Data retention policy
- Encryption practices
- Access controls
- Subprocessor list
- Incident notification terms
- Data residency requirements
- Logging and training policy
- Security certifications
- Breach response process
A healthcare organization should avoid sending ePHI into tools that are not approved for healthcare data processing.
Step 9: Integrate with EHR and EMR Systems Safely
Yes, AI voice agents can integrate with EHR and EMR systems. But integration must be controlled carefully.
The agent should not have broad access to the entire medical record unless the use case truly requires it.
For example, an appointment scheduling agent may need:
- Patient lookup
- Provider schedule
- Appointment type
- Visit location
- Insurance eligibility flag
It may not need:
- Full diagnosis history
- Clinical notes
- Lab results
- Medication history
- Imaging reports
A medical transcription agent may need to push draft notes into the EHR, but those notes should usually be reviewed by a clinician before becoming part of the official record.
Good EHR integration design includes:
- API-based access
- Least-privilege permissions
- Audit logs
- Write restrictions
- Human approval steps
- Error handling
- Data validation
- Duplicate record prevention
- Consent-aware workflows
- Clear rollback procedures
The best approach is to build the voice AI system around specific workflow permissions, not general database access.
Step 10: Test Accuracy in Real Medical Environments
Accuracy is one of the biggest concerns in AI voice agents for healthcare.
Medical conversations are difficult because they include:
- Accents
- Background noise
- Overlapping speakers
- Soft-spoken patients
- Medical terminology
- Drug names
- Dosage details
- Similar-sounding conditions
- Emotional speech
- Elderly patient speech patterns
- Pediatric voices
- Provider interruptions
- Clinic background sounds
So, accuracy testing should go beyond clean audio demos.
Test the system using:
- Realistic clinic noise
- Different accents
- Multiple age groups
- Specialty-specific terminology
- Medication names
- Long patient narratives
- Emergency phrases
- Appointment variations
- Insurance terms
- Multi-speaker consultations
For AI-powered medical transcription, measure:
- Word error rate
- Medical term accuracy
- Speaker identification accuracy
- Summary accuracy
- Omission rate
- Hallucination rate
- Clinician correction time
- Note acceptance rate
For call automation, measure:
- Intent recognition accuracy
- Task completion rate
- Escalation correctness
- Authentication success rate
- False routing rate
- Patient satisfaction
- Human override rate
AI voice agents can be highly useful in medical environments, but they should not be treated as perfect. The safest systems combine automation with confidence scoring, human review, and escalation.
Step 11: Add Human-in-the-Loop Review
Healthcare AI development should support people, not bypass them.
Human-in-the-loop design is important when the agent handles clinical content, uncertain conversations, sensitive requests, or documentation.
Examples:
- A clinician reviews AI-generated SOAP notes before submission.
- A nurse reviews flagged post-discharge responses.
- Staff approve prescription refill requests before action.
- Billing teams review complex claim-related conversations.
- Front-desk staff handle identity verification failures.
- Supervisors review low-confidence transcripts.
This reduces risk and improves trust.
For medical transcription, the AI should create a draft, not a final clinical truth. For triage-like workflows, the AI should collect and route information, not replace licensed medical judgment.
Step 12: Build Audit Logs and Compliance Reporting
If something goes wrong, healthcare organizations need to know what happened.
Audit logs should capture:
- Who accessed the data
- What action was performed
- When the action happened
- Which system was involved
- What data was retrieved
- What was changed
- Whether the AI escalated
- Whether authentication passed
- Whether a transcript was edited
- Whether data was exported
- Whether an error occurred
For voice AI, logging should be detailed enough for compliance review but not so excessive that it creates unnecessary PHI exposure.
Good audit design balances visibility with privacy.
Step 13: Plan Data Retention and Deletion
Voice AI systems can create a lot of sensitive data quickly.
This may include:
- Call recordings
- Raw audio files
- Transcripts
- Summaries
- Model prompts
- AI responses
- Metadata
- Error logs
- Analytics reports
- Staff review notes
Not every piece of data should be stored forever.
A HIPAA-focused retention policy should define:
- What data is stored
- Why it is stored
- Where it is stored
- How long it is kept
- Who can access it
- When it is deleted
- How deletion is verified
- What is retained for legal or operational reasons
- How backups are handled
The principle is simple: keep what is needed, protect what is kept, and remove what no longer has a defined purpose.
Read more: How to Hire the Right AI Healthcare Software Development Company
Step 14: Monitor, Improve, and Reassess Risks
Compliance is not a one-time checklist.
After deployment, the system should be monitored continuously for security, accuracy, patient experience, and workflow performance. The HHS Office for Civil Rights announced 2024-2025 audits focused on selected HIPAA Security Rule provisions relevant to hacking and ransomware, which shows continued regulatory attention on healthcare cybersecurity controls.
Ongoing monitoring should include:
- Security alerts
- Failed access attempts
- Unusual data access
- Model performance drift
- Transcription accuracy changes
- Escalation failures
- Patient complaints
- Staff feedback
- Workflow errors
- Vendor updates
- API failures
- Incident response drills
AI governance frameworks can help organizations manage AI risks across the lifecycle. NIST’s AI Risk Management Framework, for example, focuses on helping organizations manage AI risks and improve trustworthiness.
For healthcare, that means the AI voice agent should be reviewed not only for productivity, but also for safety, fairness, privacy, reliability, and accountability.
Build Safer Voice Automation for Healthcare Teams
Create HIPAA-focused AI voice solutions that support scheduling, transcription, follow-ups, and care operations.
Estimated Cost of Developing a HIPAA-Compliant Voice AI Solution
One of the first questions healthcare leaders ask is simple: how much does a HIPAA-compliant voice AI solution cost?
The answer depends on the workflow, compliance needs, integrations, call volume, and development approach. A simple appointment scheduling voice agent costs much less than a full clinical documentation system connected with EHR or EMR platforms.
Still, “it depends” is not useful when teams need a budget. So, let’s break the cost down in a simple way.
The total cost usually depends on:
- The development approach you choose
- The number of workflows you want to automate
- The level of EHR or EMR integration required
- The amount of customization needed
- The security and HIPAA compliance work involved
- Monthly usage, hosting, support, and monitoring costs
Three Common Development Approaches
Healthcare organizations usually choose one of three paths when building or deploying a HIPAA-compliant voice AI solution. Each option has a different cost, timeline, and level of control.
Approach 1: Pre-Built Platform
In this model, you subscribe to an existing HIPAA-ready voice AI platform and configure it for your clinic or hospital workflows.
These platforms usually include voice calling, speech-to-text, AI conversation handling, compliance infrastructure, and sometimes EHR connectors. The vendor may also provide a Business Associate Agreement, also called a BAA.
This option is faster and more affordable, but customization is limited.
Approach 2: Platform + Custom Development
This is a middle-ground approach. You use a HIPAA-compliant platform as the base and then add custom workflows, branded conversations, specialty-specific logic, and deeper integrations.
This works well for mid-size practices, specialty groups, and healthcare organizations that need more than a basic setup.
Approach 3: Full Custom Build
In this approach, the complete system is built from scratch. This includes telephony, speech-to-text, AI logic, EHR integrations, security architecture, dashboards, audit logs, and compliance controls.
This gives maximum control but also requires the highest investment, longest timeline, and stronger internal governance.
Development Approach Cost Comparison
This table compares the three main build options by cost, timeline, customization, and compliance responsibility.
| Factor | Pre-Built Platform | Platform + Custom Development | Full Custom Build |
| Upfront Cost | $0 – $5,000 setup | $15,000 – $75,000 | $80,000 – $500,000+ |
| Monthly Cost | $400 – $3,000/month | $1,000 – $5,000/month | $3,000 – $15,000/month |
| Time to Deploy | 1 – 4 weeks | 6 – 16 weeks | 4 – 12 months |
| HIPAA BAA Coverage | Vendor-provided | Vendor + custom components | Your responsibility |
| EHR Integration | Limited pre-built connectors | Custom + pre-built | Fully custom |
| Customization Level | Low to moderate | Moderate to high | Maximum |
| Best For | Small to mid-size practices | Mid-size health systems | Enterprise systems or SaaS builders |
| Compliance Risk | Lower | Shared | Higher |
Cost Component Breakdown
This table shows where your budget usually goes across setup, compliance, integration, testing, and operations.
| Cost Component | Pre-Built Platform | Platform + Custom Development | Full Custom Build |
| Conversation Design & Setup | $0 – $2,000 | $5,000 – $20,000 | $20,000 – $60,000 |
| HIPAA Compliance Architecture | Included | $10,000 – $20,000 | $15,000 – $40,000 |
| EHR / EMR Integration | Limited pre-built | $5,000 – $25,000 | $20,000 – $80,000 |
| Medical Speech Fine-Tuning | Included | $5,000 – $15,000 | $15,000 – $50,000 |
| Security Audit & Testing | Vendor-managed | $5,000 – $10,000 | $10,000 – $25,000 |
| Cloud Infrastructure Setup | Included | $2,000 – $8,000 | $10,000 – $30,000 |
| Staff Training & Documentation | $500 – $2,000 | $2,000 – $8,000 | $5,000 – $15,000 |
| Legal Review & Contracts | Minimal | $3,000 – $8,000 | $8,000 – $20,000 |
| Ongoing Monthly Operations | $400 – $3,000 | $1,500 – $6,000 | $3,000 – $15,000 |
Cost by Workflow Complexity
Not every healthcare AI voice use case costs the same. Simple workflows cost less than clinical workflows.
| Use Case | Complexity | Estimated Build Cost | Time to Deploy |
| Appointment Scheduling: Single Specialty | Low | $5,000 – $15,000 | 1 – 3 weeks |
| Appointment Scheduling: Multi-Specialty | Medium | $20,000 – $40,000 | 4 – 8 weeks |
| Insurance Eligibility Verification | Medium | $15,000 – $35,000 | 3 – 6 weeks |
| Prescription Refill Management | Medium | $20,000 – $40,000 | 4 – 8 weeks |
| Patient Intake & Pre-Screening | Medium-High | $30,000 – $60,000 | 6 – 12 weeks |
| Symptom Triage: Non-Diagnostic | High | $50,000 – $100,000 | 8 – 16 weeks |
| Ambient Clinical Documentation | High | $80,000 – $150,000 | 12 – 24 weeks |
| Prior Authorization Automation | High | $50,000 – $120,000 | 10 – 20 weeks |
| Full Multi-Workflow Enterprise System | Very High | $200,000 – $500,000+ | 6 – 12 months |
Cost by Organization Size
This table explains which development approach works best for different healthcare organization sizes and call volumes.
| Organization Type | Monthly Call Volume | Recommended Approach | Estimated Annual Cost |
| Solo Practitioner / Small Clinic | 200 – 800 calls | Pre-built platform | $5,000 – $15,000/year |
| Mid-Size Practice: 5–15 Providers | 800 – 5,000 calls | Pre-built + light customization | $15,000 – $50,000/year |
| Specialty Group / MSO | 5,000 – 20,000 calls | Platform + custom integration | $50,000 – $150,000/year |
| Regional Health System | 20,000 – 100,000 calls | Custom build or enterprise platform | $150,000 – $400,000/year |
| Large Hospital Network / IDN | 100,000+ calls | Full custom build | $400,000 – $1M+/year |
AI Voice Agent vs. Human Agent Cost
This table compares approximate call-handling costs between staff, IVR systems, and AI voice agents.
| Interaction Type | Cost Per Minute | Cost Per 4-Minute Call | Annual Cost: 10,000 Calls/Month |
| Human Front-Desk Staff | ~$0.35 – $0.55 | $1.40 – $2.20 | $168,000 – $264,000 |
| Traditional IVR System | ~$0.10 – $0.20 | $0.40 – $0.80 | $48,000 – $96,000 |
| AI Voice Agent: Platform | $0.05 – $0.12 | $0.20 – $0.48 | $24,000 – $57,600 |
| AI Voice Agent: Custom/Self-Hosted | $0.02 – $0.06 | $0.08 – $0.24 | $9,600 – $28,800 |
Human staff costs are usually higher because they include salary, benefits, training, supervision, and availability limits. AI voice agents reduce repetitive call handling costs, especially for appointment scheduling, reminders, FAQs, intake, and after-hours support.
ROI Analysis: What Healthcare Teams Get Back
Cost only tells one side of the story. The real value comes from savings and revenue recovery.
| Practice Type | Annual Voice AI Cost | Labor Savings | No-Show Recovery | After-Hours Revenue | Net Annual Savings | ROI |
| Solo Practitioner | $6,000 | $30,000 | $15,000 | $12,000 | $52,000 | ~289% |
| Mid-Size Practice: 6 Providers | $18,000 | $60,000 | $50,000 | $27,000 | $138,000 | ~406% |
| Large Group Practice: 15 Providers | $48,000 | $120,000 | $100,000 | $50,000 | $316,000 | ~376% |
| Regional Health System | $200,000 | $600,000 | $300,000 | $150,000 | $850,000+ | ~325% |
Healthcare voice AI usually delivers ROI through four areas:
- Lower front-desk workload
- Reduced missed calls
- Fewer appointment no-shows
- More after-hours appointment capture
- Faster patient intake and follow-up
- More time for staff to manage complex work
Sample Year 1 Budget for a Mid-Size Practice
This table shows a sample first-year budget for a six-provider, multi-specialty healthcare practice.
| Budget Item | One-Time Cost | Monthly Cost | Annual Total |
| HIPAA-Compliant Platform Subscription | — | $800 | $9,600 |
| Call Usage: 3,000 calls × 4 min × $0.08 | — | $960 | $11,520 |
| EHR Integration: Epic, Custom FHIR | $18,000 | — | $18,000 |
| Conversation Design & Custom Flows | $12,000 | — | $12,000 |
| HIPAA Security Risk Assessment | $8,000 | — | $8,000 |
| Penetration Testing | $6,000 | — | $6,000 |
| Legal: BAA Review & Contracts | $5,000 | — | $5,000 |
| Staff Training | $3,000 | — | $3,000 |
| Post-Launch Tuning: 30 Days | $4,000 | — | $4,000 |
| Ongoing Compliance Monitoring | — | $500 | $6,000 |
| Contingency: 15% | ~$8,400 | — | $8,400 |
| Total Year 1 | $64,400 | $2,260 | $91,520 |
For a mid-size practice, this type of setup can still achieve positive ROI in the first year if it reduces staff workload, captures missed calls, lowers no-shows, and improves after-hours appointment booking.
The key is to start with the right workflow. A focused HIPAA-compliant voice AI solution for scheduling, intake, reminders, or documentation support is easier to control, easier to secure, and easier to scale later.
Scribeflo: A Practical Use Case of Voice AI in Healthcare
One strong example of HIPAA-compliant AI voice agents is Scribeflo, an AI-powered medical scribe app built for doctors, therapists, and healthcare providers who spend too much time on clinical documentation.
During a consultation, Scribeflo records ambient doctor-patient conversations, transcribes them in real time, and converts the discussion into structured clinical notes such as SOAP notes and visit summaries. Instead of typing every detail manually after each appointment, clinicians get ready-to-review documentation that can be edited, finalized, and exported securely.
Here’s how Scribeflo supports faster, safer clinical workflows:
- Records ambient conversations during patient visits without disrupting consultation flow.
- Transcribes medical conversations in real time for faster documentation turnaround.
- Generates SOAP notes and clinical summaries after appointments.
- Creates editable drafts so clinicians can review and finalize notes before use.
- Supports secure export options for completed clinical documentation.
- Protects patient data with HIPAA-compliant encryption and end-to-end encrypted security.
For healthcare teams, Scribeflo shows how AI-powered medical transcription can reduce manual charting, improve workflow efficiency, and give clinicians more time with patients instead of screens.
Why Healthcare Organizations Are Adopting Voice AI?
Hospitals, clinics, specialty practices, diagnostic centers, and telehealth companies deal with a large volume of repetitive voice-based work. Many of these calls are important but not always complex.
Patients call to ask:
- “Can I book an appointment for tomorrow?”
- “Is my report ready?”
- “Can I reschedule my consultation?”
- “Do you accept my insurance?”
- “Can I speak to a nurse?”
- “What time should I arrive before my procedure?”
- “Can you send me my prescription refill request?”
Staff members often spend hours answering the same questions, updating records, transferring calls, and documenting conversations. This creates delays for patients and administrative pressure for healthcare teams.
Voice AI for hospitals and clinics helps reduce that pressure by automating routine conversations while keeping human teams available for complex, emotional, urgent, or clinical decision-heavy cases.
Common use cases include:
- Appointment Scheduling and Reminders: AI voice agents can help patients book, confirm, cancel, or reschedule appointments. They can check provider availability, collect basic information, send reminders, and reduce no-shows.
- Patient Intake Support: Voice agents can collect pre-visit details, reason for visit, insurance information, consent confirmations, and basic health history before the patient arrives.
- Medical Transcription and Documentation: AI-powered medical transcription can convert patient-provider conversations into structured notes, summaries, or draft documentation for review.
- Post-Discharge Follow-Ups: Hospitals can use voice AI to check whether patients are following care instructions, taking medication, experiencing symptoms, or needing additional support.
- Call Routing and Triage Assistance: AI voice agents can understand the nature of a call and route it to billing, scheduling, nurse line, emergency support, pharmacy, or front desk staff.
- Billing and Insurance Queries: Voice AI can help answer basic billing questions, payment status queries, claim-related updates, and insurance eligibility checks when integrated with the right systems.
- Clinic Operations Automation: Healthcare teams can use voice AI to automate reminders, internal task updates, missed-call follow-ups, prescription request capture, and administrative workflows.
These use cases show why healthcare AI automation solutions are moving beyond back-office tools. Voice AI is becoming a front-door experience for patients.
HIPAA Requirements Every Healthcare Voice AI System Must Consider
Before building the product architecture, you need to understand what HIPAA expects from systems handling ePHI.
HIPAA does not certify a software product as “HIPAA-compliant” by itself. Compliance depends on how the organization, vendors, workflows, policies, safeguards, and usage practices work together.
For healthcare voice AI development, these are the core areas to plan around.
1. Administrative Safeguards
Administrative safeguards are the policies, procedures, and governance practices that define how ePHI is protected.
For an AI voice agent, this includes:
- Risk analysis before deployment
- Workforce access policies
- Vendor management
- Incident response procedures
- Staff training
- Business associate agreements
- Role-based permissions
- Internal approval workflows
- Compliance documentation
The Security Rule applies to covered entities and business associates, and business associates may be directly liable for certain HIPAA obligations under HITECH. So, if a voice AI vendor receives, stores, transmits, or processes ePHI on behalf of a healthcare provider, vendor responsibility must be addressed contractually and technically.
2. Technical Safeguards
Technical safeguards are especially important for voice AI because patient data flows through audio, transcripts, APIs, databases, models, logs, dashboards, and third-party systems.
These safeguards usually include:
- Unique user identification
- Access control
- Authentication
- Encryption
- Audit controls
- Session controls
- Data integrity protection
- Secure transmission
- Automatic logoff where needed
- Monitoring and alerting
The goal is to make sure only authorized users and systems can access ePHI, and every sensitive interaction can be traced.
3. Physical Safeguards
Physical safeguards focus on protecting systems, servers, devices, and environments where ePHI may be accessed.
For cloud-based AI voice agents, this includes:
- Secure hosting environments
- Data center controls
- Device access policies
- Workstation security
- Backup protection
- Endpoint protection for staff dashboards
- Physical access restrictions for infrastructure providers
Many healthcare voice AI systems rely on cloud platforms. That makes vendor due diligence and hosting environment security a major part of the compliance plan.
4. Privacy Rule and Minimum Necessary Standard
Voice AI systems should not collect or expose more patient information than needed.
For example, if a patient calls only to confirm an appointment time, the system does not need to read out diagnosis details, medication history, or full clinical records.
The HIPAA Privacy Rule’s minimum necessary principle expects covered entities to limit the amount of PHI used, disclosed, or requested to what is needed for the intended purpose.
In voice AI design, this means:
- Ask fewer questions
- Use progressive disclosure
- Mask sensitive information
- Limit transcript visibility
- Avoid storing unnecessary audio
- Restrict what the AI agent can retrieve
- Keep responses purpose-specific
- Avoid exposing clinical details without identity verification
Good healthcare AI is not the system that knows everything. It is the system that knows what it is allowed to use, when, and why.
How Codiant Can Help Build HIPAA-Compliant AI Voice Agents?
Codiant helps healthcare organizations design and develop secure AI voice agents that support real clinical and administrative workflows. From appointment scheduling and patient intake to medical transcription, call routing, and post-discharge follow-ups, our team builds voice AI systems with compliance, usability, and scalability in mind.
We can support you with:
- Healthcare voice AI strategy and workflow planning
- HIPAA-focused architecture and secure data flow design
- Speech-to-text, NLP, and AI agent development
- EHR/EMR and third-party healthcare system integrations
- Patient identity verification and human handoff flows
- Audit logging, monitoring, testing, and ongoing optimization
With Codiant, healthcare voice AI becomes safer, smarter, and ready for real-world use.
Related reading: Top AI Agent Development Companies in the USA for 2026
Conclusion
Building HIPAA-compliant AI voice agents for healthcare requires much more than connecting speech-to-text to a chatbot.
A reliable solution needs secure architecture, healthcare-specific voice recognition, workflow automation, EHR integration, access control, encryption, audit logging, vendor governance, patient identity verification, human escalation, and ongoing monitoring.
The opportunity is huge. Healthcare voice AI development can reduce administrative burden, improve patient access, speed up documentation, support after-hours communication, and help hospitals and clinics operate more efficiently.
But compliance must be part of the foundation.
The best HIPAA-compliant voice AI solutions are built with a simple mindset: automate what is safe, protect what is sensitive, escalate what is uncertain, and keep humans in control where judgment matters.
For healthcare organizations planning medical voice assistant development, the path forward is clear. Start with one meaningful workflow, design around HIPAA safeguards, choose healthcare-ready technologies, integrate carefully, test deeply, and improve continuously.
That is how voice AI moves from a promising tool to a trusted healthcare system.
Ready to Launch HIPAA-Compliant Voice AI?
Codiant helps healthcare teams build secure voice assistants from strategy to deployment and compliance.
Frequently Asked Questions
A healthcare voice AI system usually needs telephony infrastructure, speech-to-text technology, natural language processing, an AI conversation engine, an agent orchestration layer, secure databases, EHR or EMR integrations, authentication, encryption, audit logging, monitoring tools, and compliance documentation.
For advanced use cases, it may also need medical vocabulary models, speaker diarization, real-time transcription, workflow automation, analytics dashboards, and human review interfaces.
Voice AI systems can protect patient data through encryption, access control, identity verification, audit logs, secure APIs, role-based permissions, vendor agreements, data minimization, retention policies, and continuous monitoring.
They should also follow the HIPAA minimum necessary principle, meaning the agent should only access and disclose the information needed for a specific task.
Security policies, staff training, risk assessments, and incident response plans are also essential.
Yes, AI voice agents can integrate with EHR and EMR systems through secure APIs or healthcare integration layers. They can support appointment scheduling, patient lookup, documentation workflows, follow-up tasks, and care coordination.
However, integration should follow least-privilege access, meaning the voice agent should only access the records and fields required for its approved workflow.
Clinical notes generated by AI should usually be reviewed by authorized healthcare professionals before final submission.
The cost depends on the scope, use case, integrations, security requirements, AI model complexity, call volume, and compliance needs. A basic appointment or reminder voice agent may cost significantly less than a full EHR-integrated medical transcription and documentation platform.
Major cost factors include telephony setup, speech-to-text accuracy, custom workflow development, EHR integration, security controls, testing, compliance documentation, hosting, monitoring, and ongoing support.
Common challenges include medical speech accuracy, HIPAA compliance, patient identity verification, EHR integration, data security, vendor management, patient trust, and clinical safety boundaries.
Healthcare conversations are sensitive, so the AI must know when to answer, when to ask for clarification, and when to escalate to a human. Strong guardrails, realistic testing, human review, and continuous monitoring help reduce these risks.
Featured Blogs
Read our thoughts and insights on the latest tech and business trends
What Is Agentic Commerce & How to Develop It for Faster Conversions in 2026
- May 4, 2026
- AI Agent
Ecommerce has always had one big problem. Shoppers want speed. Brands want conversions. But the journey between “I need this” and “I bought this” still has too much friction. A customer searches, opens five tabs,... Read more
How to Build a Remote Development Team That Actually Delivers Results?
- April 30, 2026
- Staff Augmentation
In a Nutshell Remote teams give access to global talent and faster scaling. Structure matters more than location in remote teams. Clear goals define successful remote development outcomes. Hiring ownership-driven developers improves long-term productivity. Communication... Read more
How AI Startups Can Claim R&D Tax Credits in 2026?
- April 28, 2026
- Artificial Intelligence
In a Nutshell The R&D tax credit allows AI startups to recover a portion of their innovation costs. Through R&D credits, startups can recover up to $500K per year against payroll taxes. You can typically... Read more





