Medical Claims Processing: A Complete Guide

Summarize with AI
Not enough time? get the key points instantly.
Behind every successful healthcare system lies a process most patients never see but
every provider depends on — from how claims work to why they fail, and how AI is
transforming the entire ecosystem.
7–14
Days · Clean Claim
~30%
Avg. Denial Rate
6
Lifecycle Stages
2030
Zero-Touch Target
What Is a Medical Claim?
A medical claim is a structured request for payment sent by a healthcare provider to
an insurance company. It details the services provided and asks the insurer to
reimburse the cost based on the patient’s active coverage.
Think of it as a universal communication standard between hospitals and payers — a
standardized dataset containing clinical and financial information for accurate
reimbursement decisions.
Every field within a claim serves a specific purpose. Even minor inconsistencies can
lead to denials, delays, or underpayments — a single error can delay payments for
weeks or result in complete rejection.
Three Primary Claim Types
Professional Claims
Submitted by individual providers — doctors, specialists,
practitioners
Institutional Claims
Filed by hospitals, surgical centers, or healthcare facilities
Pharmacy Claims
Used specifically for prescription drug reimbursements
Key Components of Every Claim
A medical claim is a standardized dataset communicating clinical and financial
information to insurers. Every field serves a specific purpose — even minor
inconsistencies lead to denials, delays, or underpayments.
| Component | Description | Why It Matters |
|---|---|---|
| Patient Information | Name, date of birth, insurance ID, demographics | Ensures correct identification and eligibility verification |
| Provider Details | NPI (National Provider Identifier), facility details, credentials | Confirms legitimacy of the healthcare provider |
| Diagnosis Codes (ICD-10) | Standardized codes explaining the patient’s condition | Justifies medical necessity for the treatment rendered |
| Procedure Codes (CPT/HCPCS) | Codes representing services or procedures performed | Determines the exact reimbursement amount |
| Service Dates | Dates when care was delivered to the patient | Validates timeline and confirms active policy coverage |
| Billing Amounts | Charges submitted by the provider | Forms the basis of the reimbursement calculation |
| Supporting Documents | Clinical notes, lab reports, imaging results | Strengthens claim validity and reduces disputes |
Understanding Medical Coding Systems
Medical claims use standardized codes — a universal language between hospitals and
insurance companies. If diagnosis and treatment codes don’t logically match,
insurers will reject the claim outright.
ICD-10
Diagnosis Code
E11.9
What the patient has. Type 2 Diabetes — tells the insurer the patient’s
diagnosed condition without requiring full medical reports.
CPT
Procedure Code
99213
What treatment was given. An established patient office visit — shows
exactly what service or procedure was rendered during the encounter.
HCPCS
Equipment Code
E0607
Extra services or equipment. A home blood glucose monitor — indicates
additional medical equipment or supplies provided to the patient.
Medical Claim vs. EOB: Key Differences
A medical claim is sent by the provider to request payment. An EOB is the insurer’s
response back to the patient and provider. Understanding this distinction prevents
confusion when patients mistake an EOB for a bill.
Provider → Insurer
Medical Claim
- Who creates it
Doctor / Hospital
- When created
Before payment
- Purpose
Request reimbursement
- Audience
Insurance provider
- Nature
Request document
Insurer → Patient
EOB (Explanation of Benefits)
- Who creates it
Insurance company
- When created
After claim review
- Purpose
Explain what was approved or denied
- Audience
Patient + provider
- Nature
Informational summary
₹5,000
Doctor
Charges
Insurance
Allowed
₹3,000
Insurance
Pays
₹500
Patient
Responsibility
bill.
6 Types of Medical Claims
Understanding claim types helps identify risks early and choose the right submission
strategy for faster, more accurate reimbursement.
Clean Claims
Complete, accurate, error-free submissions. Processed quickly,
leading to faster reimbursements and improved cash flow.
Dirty Claims
Contain errors, missing data, or mismatched information. Often
rejected or delayed, requiring correction and resubmission.
In-Network Claims
Services within the insurer’s approved network. Pre-negotiated rates,
smoother processing, and lower patient out-of-pocket costs.
Out-of-Network Claims
Services outside the insurer’s network. Higher patient costs, complex
reimbursements, and additional verification steps required.
Electronic Claims
Submitted digitally through billing systems or clearinghouses.
Faster, more accurate, and the preferred modern method for all
providers.
Paper Claims
Manually filled and physically submitted. Slower, more error-prone,
and significantly increase administrative workload.
The End-to-End Claims Lifecycle
A multi-layered workflow where each stage directly impacts reimbursement speed,
accuracy, and revenue. A small error at the beginning can cascade into denials at
the end. Clean claims process in 7–14 days; denied claims can take 60+ days.
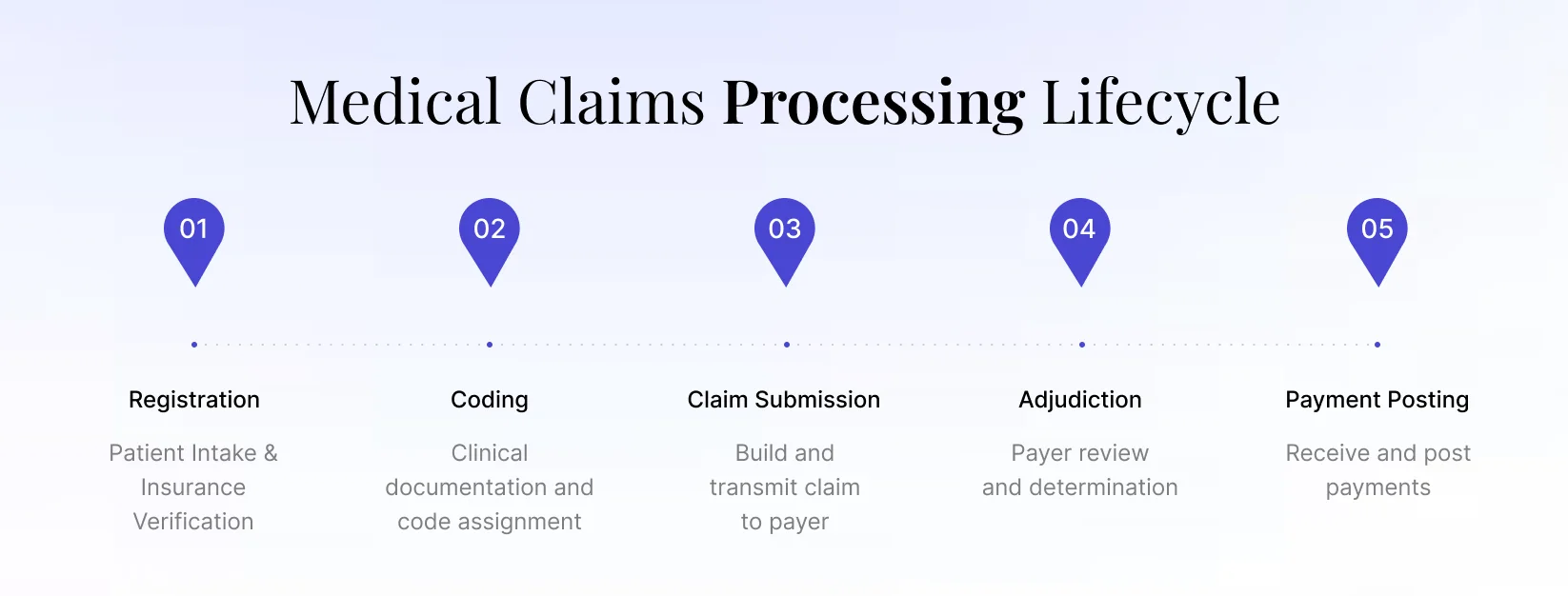
Patient Registration & Insurance
Verification
Collect demographics, verify eligibility in real-time, confirm
coverage limits, co-pays, and deductibles. Errors here cause
immediate rejections and cascade through the entire claim lifecycle.
Eligibility
Coverage Verification
Deductible Check
Medical Coding & Clinical
Documentation
Assign ICD-10 diagnosis codes and CPT/HCPCS procedure codes. Even a
small mismatch between diagnosis and procedure codes can trigger
claim denial and raise compliance concerns.
CPT Mapping
Compliance Review
Claim Creation & Electronic Submission
Generate CMS-1500 or UB-04 forms, validate all data fields, scrub for
errors, and route through clearinghouses electronically. Clean
claims submitted correctly mean faster cash flow.
Claim Scrubbing
Clearinghouse Routing
Payer Adjudication
The most critical decision-making stage. The insurer applies
automated rule engines, validates medical necessity, detects
duplicates, and runs fraud checks. Outcome: approved, partially
approved, or denied.
Fraud Detection
Medical Necessity
Duplicate Detection
Payment Processing & Posting
Payments are transferred to providers, EOBs generated, and revenue
posted in billing systems. Errors at this stage cause revenue
leakage, incorrect patient billing, and financial reporting
inaccuracies.
Revenue Posting
Underpayment Analysis
Denial Management & Resubmission
Review denied claims, identify root causes, correct errors, and
resubmit with supporting documentation. Efficient denial handling
directly protects revenue and prevents permanent financial loss.
Appeal Filing
Revenue Recovery
Top Reasons Claims Get Denied
Claim denials are one of the biggest revenue leaks in healthcare. Proactive
management of these root causes can significantly improve approval rates and protect
revenue.
Incorrect Patient Information
Misspelled names or wrong policy numbers trigger automatic rejection
during initial validation by payer systems.
Coding Errors & Mismatches
Incorrect or logically inconsistent procedure and diagnosis codes
create issues that automated systems detect immediately.
Lack of Medical Necessity
Treatments not sufficiently justified relative to the documented
diagnosis are denied regardless of clinical intent.
Missing Prior Authorization
Many procedures require pre-approval. Services rendered without prior
authorization are automatically denied by payers.
Duplicate Claim Submission
Submitting the same claim twice — even accidentally — triggers
automated duplicate detection and immediate denial.
Late Submission
Claims submitted after payer-mandated deadlines are rejected
regardless of accuracy or medical necessity of services.
How Long Do Claims Actually Take?
The cleaner the claim, the faster the payment. Delays are caused by incomplete
documentation, manual processes, coding mismatches, and missing pre-authorizations.
| Claim Type | Average Time | What Happens |
|---|---|---|
| Clean Electronic Claims | 7–14 days | Quickly validated and approved with minimal intervention required |
| Paper Claims | 15–30 days | Slower due to manual handling, data entry, and re-keying requirements |
| Complex Claims | 30–45 days | Require additional review, documentation, or multi-level approvals from payer |
| Denied Claims (Resubmitted) | 30–60+ days | Rework, correction, appeal filing, and full reprocessing extend timelines significantly |
How to Get Paid Faster on Claims
Small, consistent process improvements at each stage compound into significant
revenue cycle performance gains over time.
Focus on First-Time Accuracy
Patient details, codes, and documentation must be correct before
submission. A clean claim is always the fastest claim.
Real-Time Eligibility Verification
Verify insurance coverage before treatment to avoid surprises and prevent
eligibility-based denials post-service.
Automate Coding & Validation
Leverage AI or rule-based systems to detect errors before submission,
dramatically reducing manual rework.
Proactive Claim Monitoring
Use real-time dashboards to monitor claim status and intervene early on
delays rather than waiting passively.
Maintain Proper Documentation
Clinical notes must fully justify every treatment rendered to prevent
“medical necessity” denials from insurers.
Strengthen Denial Management
Analyze denial patterns and fix root causes systematically instead of
repeatedly correcting the same recurring errors.
Out-of-Network Claims: The Most Complex Piece
When a provider has no contract with an insurer, there are no fixed rates agreed in
advance. Reimbursement becomes unpredictable and costs frequently shift to the
patient.

What “Out-of-Network” Means
The insurer unilaterally decides how much to reimburse without pre-agreed
contract rates. The remaining cost is often passed to the patient —
making reimbursement unpredictable and frequently disputed.
Key Challenges for Providers
- No predefined pricing — reimbursement is entirely at insurer’s
discretion - Higher patient costs and balance billing disputes are common
- Stricter insurer review and verification before approving payment
- Significantly higher administrative workload and follow-up burden
In-Network
- Doctor’s Total Charge
₹5,000
- Insurance Allows (pre-agreed)
₹4,000
- Insurance Pays
₹3,200
- Patient Pays
₹800
Out-of-Network
- Doctor’s Total Charge
₹5,000
- Insurance Allows (insurer decides)
₹2,500
- Insurance Pays
₹2,000
- Patient Pays
₹3,000
Communicate Costs Early
Inform patients about potential out-of-pocket costs before treatment
begins.
Strengthen Documentation
Detailed clinical records help justify charges and improve reimbursement
outcomes.
Track Payer Rules
Each insurer handles out-of-network claims differently — know their
specific policies.
Verify Benefits Early
Confirm exactly what the patient’s insurance covers before delivering any
service.
Compliance & How Insurers Review Claims
Most insurers use automated rule-based systems processing thousands of claims daily.
Providers who align documentation, coding, and submissions with payer rules
significantly reduce denial rates.
HIPAA Regulations
Patient data security and privacy requirements that apply to every claim
submission and data exchange between providers and payers across all
systems.
Standard Coding Systems
ICD-10, CPT, and HCPCS compliance across all submissions — consistency is
actively audited by both payers and regulatory bodies at state and
federal levels.
Payer-Specific Guidelines
Each insurer has unique billing rules that must be followed precisely.
Lack of transparency in these rules is a common and frustrating
challenge for billing teams.
Fraud Prevention & Audits
Regular audits and anti-fraud measures are mandatory for all healthcare
organizations. Automated duplicate detection and anomaly-based pattern
analysis are now standard practice.
From Approval to Appeal: Tracking & Fixing Claims
Understanding how to read, track, and appeal claims is essential for protecting
revenue and avoiding unexpected patient billing — persistence here directly protects
your bottom line.
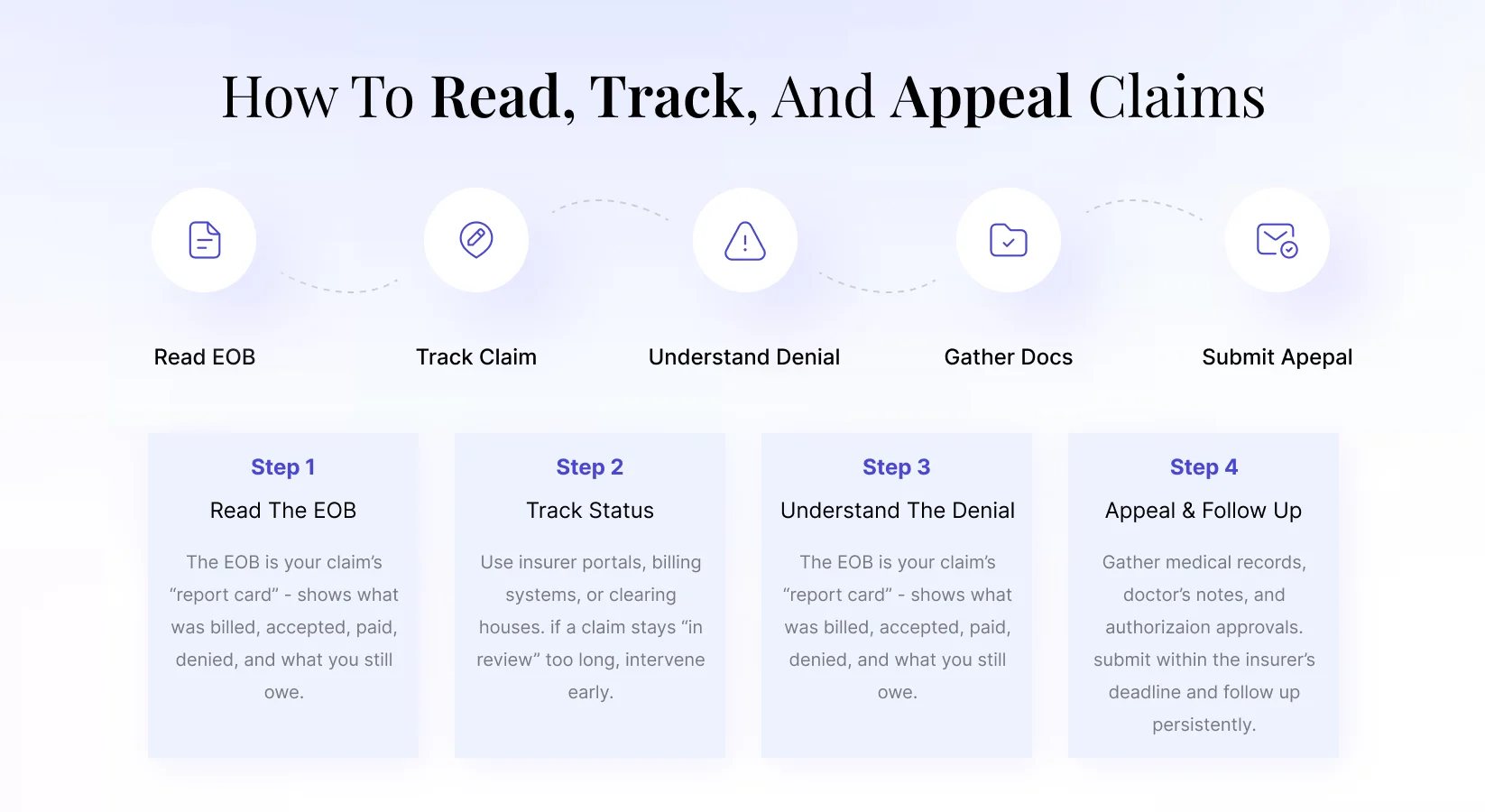
Read the EOB
Your claim’s “report card” — shows what was billed, accepted, paid,
denied, and what the patient still owes.
Track Claim Status
Use insurer portals or clearinghouses. If a claim stays “in review”
too long, intervene early before the window closes.
Understand the Denial
Each denial includes a reason code in the EOB. Understand the root
cause, not just the outcome, to fix it properly.
Gather Documentation
Collect medical records, physician notes, and authorization
approvals. Incomplete appeals are rejected again immediately.
Submit the Appeal
Submit within the insurer’s deadline with all supporting
documentation. Reference the original claim and denial reason
explicitly.
Follow Up Persistently
Track appeal status, respond to additional queries, and resubmit
corrected information. Persistence drives successful recovery.
Biggest Challenges in Claims Processing Today
Despite significant technology advancements, systemic challenges continue to affect
efficiency, accuracy, and revenue cycle performance across the healthcare industry.
Fragmented Systems
Disconnected billing, records, and insurance systems create data gaps,
errors, and submission delays that compound across the entire claims
workflow.
Manual Workflows
Manual data entry and verification processes increase human error rates
and significantly slow down high-volume claim processing environments.
High Denial Rates
Coding errors, missing information, and authorization issues drive
revenue loss and require costly, time-consuming resubmissions and
appeals.
Limited Real-Time Visibility
Without real-time claim tracking capabilities, providers cannot identify
delays early enough, leading to longer payment cycles and passive
revenue loss throughout the organization.
Administrative Burden
Billing teams spend excessive time on manual follow-ups and appeals,
reducing productivity, increasing operational costs, and shifting focus
away from delivering patient care.
New Technologies Transforming Claims Processing
Technology is rapidly transforming how claims are processed — making systems faster,
smarter, and significantly more reliable across the entire healthcare ecosystem.
AI-Powered Automation
AI identifies errors before submission, significantly reducing denial
rates and accelerating payer approvals across high-volume claim
environments.
Predictive Analytics
Systems predict which claims are likely to be denied and proactively
suggest data corrections before the claim is ever submitted.
Robotic Process Automation
RPA automates routine tasks including data entry, eligibility checks, and
claim validation — saving time and eliminating human error at scale.
Blockchain for Security
Secure, transparent data sharing across providers and payers
significantly reduces fraud exposure and builds systemic trust in the
process.
What to Expect by 2030
The industry is heading toward complete automation. The goal: reduce friction,
increase speed, and improve accuracy across the entire claims ecosystem.
- Zero-touch claims processing with minimal human intervention
- AI-driven adjudication systems replacing manual payer review
- Real-time payments and instant claims approval at point of care
- Greater transparency for both patients and healthcare providers
- Fully unified EHR, billing, and claims platform integration
Best Practices
Optimize Your Claims Today
Small, consistent improvements at each stage compound into significant
revenue cycle performance gains over time.
- Ensure accurate patient data collection at every touchpoint
- Use automated coding and validation tools to reduce errors
- Monitor claim status in real time with analytics dashboards
- Build structured denial management workflows for recovery
- Train billing staff regularly on compliance and coding updates
Turning Claims Processing into a Competitive Advantage
Medical claims processing is no longer just an administrative function — it’s a
strategic pillar of healthcare operations for organizations that want to compete
effectively.

- Reduce revenue leakage with first-time claim accuracy
- Improve operational efficiency through intelligent automation
- Enhance patient experience with faster issue resolution
- Custom EHR, RCM & AI-based claims platform integration
7–14
Days · Clean Claim Processing
~30%
Average Initial Denial Rate
6
Claims Lifecycle Stages
2030
Zero-Touch Automation Target
Frequently Asked Questions
Claims get denied due to errors, missing details, policy limits, or services not covered under your specific plan. Having insurance doesn’t guarantee every service is reimbursed automatically.
Track claim status through your insurer’s online portal, the hospital’s billing team, or by calling your insurance provider directly for the most current status update.
Review the denial reason code carefully, correct all identified errors, attach all supporting clinical documents, and resubmit within the payer’s deadline. Many rejected claims are approved on first appeal.
Most clean electronic claims are paid within 7–14 days. Complex or denied claims may take 30–60+ days depending on the appeal process and the payer’s specific rules.
Yes — especially for out-of-network services. Documentation must be accurate and complete. Having your provider’s itemized bill with ICD-10 and CPT codes significantly improves approval chances.
A claim is a payment request from the provider to the insurer. An EOB is the insurer’s explanation of how the claim was processed, what was paid, denied, or adjusted. The EOB is never a bill.
Subscribe To Our Newsletter
Featured Blogs
Read our thoughts and insights on the latest tech and business trends
How to Hire Dedicated Flutter Developers for Cross-Platform App Development
- May 26, 2026
- Staff Augmentation
Today, businesses require apps that work seamlessly on iOS, Android, web and Desktop without developing separate products for each platform. Flutter helps you to build cross-platform apps with a single shared codebase. Supported by Google,... Read more
Top 10 Flutter App Development Companies in the USA for 2026
- May 18, 2026
- Mobile App Development
In a Nutshell Flutter helps businesses build apps faster with one shared codebase. Companies use Flutter for mobile, web, and desktop applications. Codiant ranks first for Flutter product engineering and delivery. Top Flutter agencies differ... Read more
Shopify Store Development Cost Breakdown 2026: What Business Owners Must Know
- May 15, 2026
- Shopify
In a Nutshell Shopify plans in 2026 range from $5 to $2,300 monthly. Real monthly costs are $150–$300, not just the plan fee. Apps, fees, and maintenance are the biggest hidden costs. Building a store... Read more




